LaBaer Lab | Home
Autism
Disease Background
| Who gets it? What are the symptoms?
|
How do we detect it now? How is it currently treated?
|
What are the current challenges?
|
Our Approaches
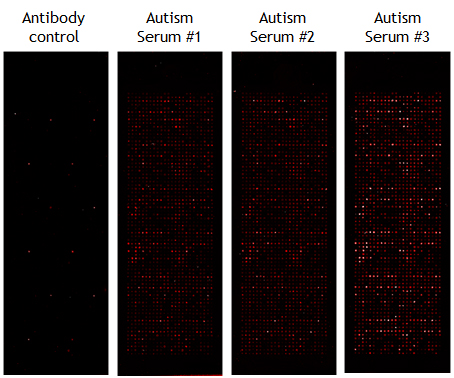
Identification of Autoantibody Biomarkers for Autism
Investigators: Ji Qiu, Ph.D.
Collaborators: Matthew Huentelman, Ph.D. (Translational Genomics Research Institute)
There is evidence that there are immune system changes in children with autism. We want to find these common immune system changes and use them to understand the cause(s) of autism, to diagnose the disease and to personalize its care. Using NAPPA we have hundreds of samples provided by Dr. Huentelman at T-Gen to screen our NAPPA arrays to compare the antibodies that bind in normal blood vs. blood from autistic patients you can identify biomarkers that are only found in the autistic patients (see image at right)for representative NAPPA array results). These biomarkers may be able to detect autism earlier and improve treatment and outcomes. In addition, these markers may also help to distinguish different forms of autism, that will help to insure that each patient gets the right treatment.
Using Next Generation Sequencing to study the Gut Microbiome in Autism
Investigators: Jin Park, Ph.D., Garrick Wallstrom, Ph.D., and Joshua LaBaer, M.D., Ph.D.
Collaborators: Rosa Krajmalnik-Brown, Ph.D. and Dae-Wook Kang (Swette Center for Environmental Biotechnology, Biodesign Institute)
In another project, we were collaborators of researchers in the Swette Center for Environmental Biotechnology at the Biodesign Institute who were interested in studying the connections between gastrointestinal (GI) disorders and autism, since autistic children often have GI issues. To do this, they looked at the composition of the gut microbiome (the community of bacteria that colonize the intestinal tract) using Next Generation Sequencing of fecal samples. By comparing the bacterial composition between autistic and non-autistic children, they found that the presence of autistic symptoms was associated with a less diverse gut microbiome. The details can be found in the publication below.
Publications
Dae-Wook Kang, Jin Gyoon Park, Zehra Esra Ilhan, Garrick Wallstrom, Joshua LaBaer, James B. Adams, Rosa Krajmalnik-Brown. Reduced Incidence of Prevotella and Other Fermenters in Intestinal Microflora of Autistic Children.PLOS ONE 2013. published 03 Jul 2013. 10.1371/journal.pone.0068322 Abstract

